How to choose personal protective equipment
What is personal protective equipment?
Personal protective equipment (PPE) includes gloves, gowns, masks, face shields, goggles, shoe covers and head covers. Wearing PPE in the hospital and medical clinics/offices helps prevent the spread of germs and protects both patients and health care workers from infection.
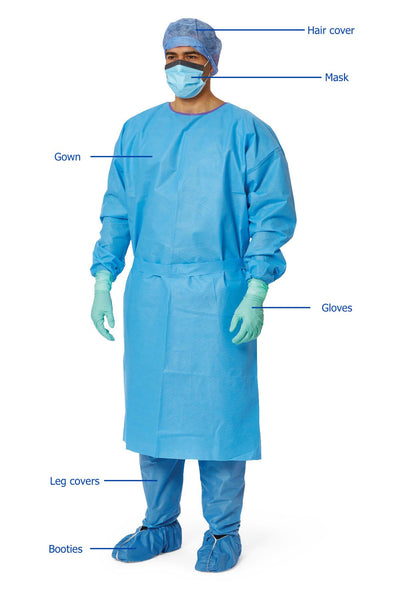
Protecting your hands
Examination gloves create a barrier between germs and your hands. Wearing gloves helps keep your hands clean and lessens your chance of getting germs that can make you sick.
Wear gloves every time you touch blood, bodily fluids, bodily tissues, mucous membranes, or broken skin. Even if a patient seems healthy and has no signs of any germs, you should still wear gloves.
Surgical gloves are sterile and offer higher level of protection than examination gloves, as well as higher sensitivity needed for delicate surgical work.
Consult this link to learn more about choosing the right gloves.
Protecting your lungs
There are 3 main types of masks:
-
Procedure masks have two ear loops to secure the mask to the face. You can use these on hospital floors, in isolation units and labor and delivery units. Additionally, these masks are suitable for emergency departments and the intensive care units for bedside procedures. However, they are not sufficient for use in the operating room.

-
Surgical masks are designed for sterile areas, such as the operating room. These masks have two straps, instead of loops, that secure the mask to the face. Some surgical masks have anti-fog features that keep your glasses or goggles from fogging up. Surgical masks are also made to protect against a high risk of fluid exposure.

-
N95 respirator can filter surgical smoke created by electrosurgical units, lasers and ultrasonic scalpels or dissectors during invasive procedures. This type of mask is also suitable for higher-risk aerosol-generating procedures on patients with known or suspected aerosol-transmittable diseases such as tuberculosis, varicella and rubella. Standard surgical masks are insufficient in these cases.

Protecting your eyes
The eye protection equipment requirements depend on the kind of exposure, other PPE used, and personal vision needs. The most important factor in protective eyewear selection is the nature and extent of the hazard. Eye protection must also be comfortable, allow for good peripheral vision and adjustable to ensure a secure fit.
Goggles
Properly fitted, indirectly-vented goggles with a manufacturer’s anti-fog coating provide the most reliable eye protection from splashes, sprays, and respiratory droplets. Many styles of goggles fit well over prescription glasses with minimal gaps. To be effective, goggles must fit snugly, particularly from the corners of the eye across the brow. While highly effective as eye protection, goggles do not provide splash or spray protection to other parts of the face.

Face Shields
Face shields are an infection control alternative to goggles. Compared with goggles, a face shield can also protect facial areas other than eyes. For better face and eye protection from splashes and sprays, a face shield should have crown and chin protection and wrap around the face to the point of the ear. This will reduce the likelihood of splash traveling around the edge of the shield and reaching the eyes


Safety Glasses
Safety glasses provide impact protection but do not provide sufficient splash or droplet protection. Generally, you should not use safety glasses for infection control purposes; use goggles instead.
Protecting your head
Recently, an argument erupted between the proponents of a surgical skull cap and a bouffant cap. Male surgeons strongly prefer the skull cap, but the proponents of a bouffant cap state that a bouffant cap covers more hair and skin for better infection control.
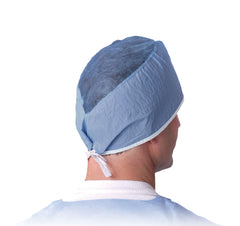

The debate is not settled, but one thing is clear. Properly fitted and appropriately worn headgear is an excellent infection prevention measure.
One of the new head covers that looks "manly" and has increased protection is a surgeon's hood.

Protecting your clothes and skin
The procedure or medical gown is the main method of protecting your clothes and skin from infection. With the help of ANSI/AAMI guidelines, the Food and Drug Administration established the gold standard for protection barrier levels all gown manufacturers must meet.
Barrier levels are based on potential exposure to blood, bodily fluids and other potentially infectious materials. The classification of barrier protection levels range from one to four and are based on the hierarchy of risks.
The hierarchy ranks medical procedures by exposure risk, accounting for the type and volume of fluid involved in the procedure, and the duration of exposure. FDA evaluates the gown material's resistance to water and blood penetration for four different areas of the gown — the front chest, sleeve seam, sleeve and front belt.
Here are the 4 barrier levels:
Level 1: Minimal risk, to be use used, for example, during basic care, standard isolation, cover gown for visitors, or in a standard medical unit;
Level 2: Low risk, to be use used, for example, during blood draw, suturing, in the Intensive Care Unit (ICU), or a pathology lab;
Level 3: Moderate risk, to be use used, for example, during arterial blood draw, inserting an Intravenous (IV) line, in the Emergency Room, or for trauma cases;
Level 4: High risk, to be use used, for example, during long, fluid intense procedures, surgery, when pathogen resistance is needed or infectious diseases are suspected (non-airborne).
Of note, all surgical gowns must be so labeled and are suitable for any risk level (1 to 4)

Protecting your feet
When considering shoe covers, the factors to evaluate are:
- Fluid resistance
- Dry surface traction (slip resistance)
- Wet surface traction
- Area of coverage


